The Effects of the Korean Medicine Health Care Program on Stroke-Related Factors and Self-Care Enhancement
Article information
Abstract
Objectives
This study was performed to examine the effects of the Korean medicine healthcare program on stroke-related factors and self-care enhancement.
Methods
This study was a quasi-experimental, pretest-posttest nonequivalent control group design study (N = 58 participants), with 28 in the treatment group (Korean medicine health care program) and 30 in the control group (no intervention). The program was conducted twice a week for 2 hours, for a total of 12 weeks.
Results
There were statistically significant differences in systolic (p = 0.005) and diastolic blood pressure (p = 0.006), cholesterol (p < 0.001), blood glucose (p < 0.001), self-esteem (p = 0.001), self-efficacy (p < 0.001), health perception (p < 0.001), and the health behavior (p < 0.001) between the experimental group and the control group.
Conclusion
Thus, the Korean medicine healthcare program was effective in managing stroke-related factors and enhancing self-care, and should be actively used to develop community health promotion strategies to prevent strokes and prepare long-term measures.
Introduction
Among the top 10 causes of death in Korea, cerebrovascular diseases are the third leading cause of death in both men and women, and account for 45.8% of the total number of deaths [1]. Stroke refers to all neurological symptoms of brain damage. Stroke risk factors include high blood pressure (BP), diabetes, dyslipidemia, heart disease, obesity, metabolic syndrome, and degenerative changes due to aging [2]. The aging population in Korea is growing at a rapid rate, in which the population aged over 65 is expected to represent 24.3% of the total population by 2030 [1]. Thus, strokes will be a major condition that will threaten health in the general population. Moreover, the incidence of strokes has increased among younger age groups (between 2010 to 2015), and the incidence of people having strokes in their 40s increased by 65% [3].
The risk of having a stroke is considered a lifestyle choice because the risk factors can be mitigated by daily management. The main causes of strokes are obesity, high BP, diabetes, and hyperlipidemia, conditions which are increasing due to unhealthy dietary changes and insufficient exercise [4]. Efforts to detect and manage adjustable stroke risk factors such as high BP, diabetes, heart disease and obesity, hyperlipidemia, smoking, excessive drinking, and insufficient exercise are essential in the prevention of cerebral infarction [2]. In particular, high BP has the highest prevalence among the adjustable risk factors and has a strong correlation with the incidence of strokes. Thus, controlling BP can reduce the incidence of strokes [5]. Diabetes is reported as an independent risk factor for ischemic strokes, and diabetic patients of the same age were reported to have a 1.8 to 6 times higher frequency of ischemic strokes than non-diabetic patients [6]. Increases in total cholesterol and low-density lipoproteins are related to ischemic strokes in both men and women. Therefore, in this study BP, blood glucose, and cholesterol were monitored as stroke risk factors.
People who are not active are 2 to 3 times more likely to experience frequent cerebral hemorrhages than active people. Moderate exercise for 30 minutes each day can lower BP and prevent strokes [6]. However, it is not easy to change lifestyle habits to include exercise, eat healthily, and control weight. Bandura [7] proposed that to be successful, there needs to be personal motivation of how to plan and implements changes in behavior. He further proposed that mastery experience, vicarious experience, and verbal persuasion are factors that can enhance self-efficacy. Moreover, self-efficacy serves as a link between health knowledge and actual behavior. Health-promoting behavior is closely related to self-efficacy [8]. Based on this relationship, studies have been performed to identify the correlation between the risks related to strokes and health-promoting behavior, through stroke prevention education programs [4]. That is, the self-esteem and self-efficacy toward oneself are expected to change the perception and behavior of health in order to continue managing stroke risk factors.
Recently, the cause of strokes was reported to be 5.1 times more frequently cited as a result of cerebral infarction, which blocks the blood vessels that supply blood to the brain causing ischemia, compared with hemorrhagic strokes where the blood vessel leaks blood [9]. The majority of strokes occur suddenly without any warning, and may lead to death or permanent disabilities if not treated promptly. Where a stroke has occurred, 70% to 75% of patients suffer from various disorders involved with movement, sensory perception, cognition, and language [9]. Stroke patients also experience further limiting effects on their daily lives, and need continuous rehabilitation for the prevention of further strokes. Many rehabilitation specialists report that patient motivation is the most important factor in the outcome of rehabilitation [10], and self-esteem is the most influential factor in rehabilitation motivation. High self-esteem encourages rehabilitation motivation [11].
In Korea, traditional Korean medicine is used by patients and their guardians, to treat symptoms of a stroke rather than Western medicine [12]. It has been shown that traditional Korean medicine is positively perceived as therapeutic [13], and has been used as a resource for health-promoting behaviors and lifestyles, in daily life to reduce stroke prevalence. Moreover, the satisfaction level of patients using Korean medicine was high (77.2%) for inpatient and (81.9%) for outpatient services [14]. Pilot projects that began in 2001 to promote health through Korean medicine have been centered around local communities to use resources effectively, improve treatment effects, and reduce national health costs. This pilot project initiative developed into the Korean medicine health promotion hub community health center project, which performs specialized local projects to meet local demands. Since 2013, health promotion policies that focus on vulnerable groups according to disease and lifestyle have been implemented through integrated community health promotion projects [15]. Whilst projects to prevent strokes and musculoskeletal diseases have also been carried out, there is a lack of research on the preventive effects of such diseases [16].
Therefore, it is necessary to review the effects of Korean medicine programs on disease types to plan respective prevention programs, and implement interventions. As Korean medicine intervention programs for local residents are widely used to prevent strokes, the purpose of this study was to examine the effects of the Korean medicine healthcare programs on stroke-related factors (BP, blood glucose, and cholesterol), self-esteem, and self-efficacy. This data may enable community health promotion policies to manage stroke-related factors, and help to provide accurate information to healthcare providers and educational resources regarding the beneficial effects of Korean medicine.
Materials and Methods
1. Research design
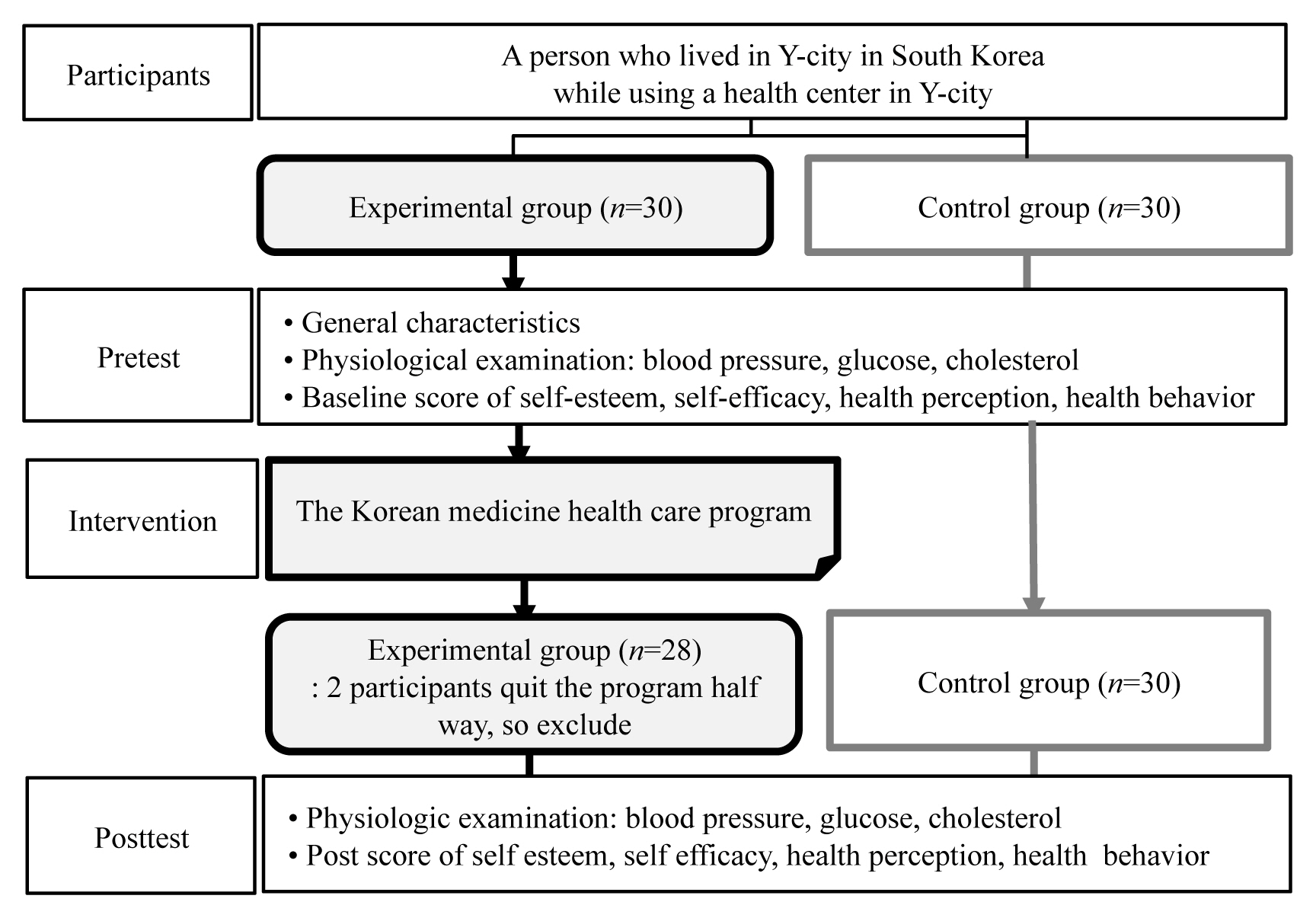
This study was a quasi-experimental design, using a pretest-posttest nonequivalent control group, to examine the effects of the Korean medicine healthcare program on stroke-related factors, self-esteem, self-efficacy, health perception and health behaviors (Figure 1).
2. Participants
The study was performed after explaining its purpose to the head and manager of the Y-city health center and the participants of this study who gave written consent. The participants were local residents who use the health center in Y-city and had chronic diseases such as high blood pressure and diabetes, or those who were interested in preventing strokes and wanted to participate in the Korean medicine healthcare program. A total of 60 participants were selected for this study and assigned to either a treatment group (participated in the Korean medicine health care program, n = 30), or control group (did not participate in the Korean medicine health care program, n = 30). However, as 2 of the treatment group participants left the program halfway, the total number of participants was 58.
The number of participants to power this study was 52 as required by ANCOVA. This was calculated using the G*Power 3.1 program set at a level of significance of 0.05, a power of 0.80, an effect size of 0.40, for 2 groups, and a dropout rate of 20%. A total sample of 58 participants was deemed appropriate.
3. Ethical consideration
This study was approved through the review process of the Bioethics Deliberation Committee of Yeongsan University (IRB approval no.: YSUIRB-201805-HR-038-02).
4. Measurements
4.1. BP, glucose, cholesterol
BP, glucose and cholesterol were measured with stroke-related risk factors. BP was measured after allowing participants to relax for at least 10 minutes. BP was measured using a mercury sphygmomanometer (Baumanmeter, NY, USA) by wrapping the cuff at the height of the heart, on the right upper arm, and the average BP was used after more than 2 measurements. Caffeine intake, exercise, and smoking 30 minutes before measuring the BP was prohibited. Fasting (≥ 8 hours) blood glucose and cholesterol levels were measured using a blood lipid measuring instrument (VERI-Q MULTI MMD-1BL, MC, KOREA): lipid/hemoglobin/glucose measuring instrument). Both concentrations were measured after participants had fasted, not participated in intense exercise or consumed alcohol within 24 hours.
4.2. Self-esteem
Self-esteem refers to respecting oneself and the evaluation of one’s own worth. This study used the self-esteem measurement tool developed by Rosenberg and Simons [17] and modified by Jeon [18]. The tool consists of 10 questions using a Likert scale. The total sum of points resulted in a minimum of 10 points and a maximum of 50 points where the higher the score the greater the indication of high self-esteem. The Cronbach’s α score was 0.84 at the time of development, and was 0.845 in this present study.
4.3. Self-efficacy
Self-efficacy refers to an individual’s belief in their capacity to succeed in organizing and implementing actions under specific circumstances [7]. This study used the tool developed by Chen et al [19] and adapted by Noh and Lee [20]. The tool consisted of 8 questions using a Likert scale. The total sum of points resulted in a minimum of 8 points and a maximum of 40 points, such that the higher the score, the higher the level of self-efficacy. The Cronbach’s α score was 0.83 when the tool was adapted by Noh and Lee [20], and was 0.917 in this current study.
4.4. Health perception and health behavior
The health perception tool used in this study was the same as the tool used for the Korean medicine health promotion project of the Ministry of Health and Welfare [15]. The tool consisted of 7 questions regarding health awareness, actions to solve health problems, health problems and lifestyle, exercise, dietary habits, and weight control. The tool used a Likert scale. The total sum of points resulted in a minimum of 7 points and a maximum of 35 points, the higher the score indicated a greater perception of health. The Cronbach’s α score was 0.873 in this current study.
The tool used in the Korean medicine health promotion project of the Ministry of Health and Welfare [15] to measure health behavior, was also used in this current study. The tool consisted of 8 questions regarding sleep, dietary habits, exercise, drinking, smoking, and weight control. The tool used a Likert scale. The total sum of points resulted in a minimum of 8 points and a maximum of 40 points, with higher scores indicating more positive behavior toward health. The Cronbach’s α score was 0.759 in this current study.
5. Data collection
Data were collected from May, 2018 to October, 2018. When participants filled out the questionnaire, they also provided their date of birth, and phone number. This information was used to match the pre- and post-examination data.
The pretest was conducted to examine the general characteristics of the participants, and to measure baseline BP, glucose, cholesterol, and filled out questionnaire to self-esteem, self-efficacy, health perception and health behavior. The pretest was completed before starting the study (in the 1st week), and the posttest was performed after completion of the program (the same methods of measurement were used as the pretest).
6. Implementation program
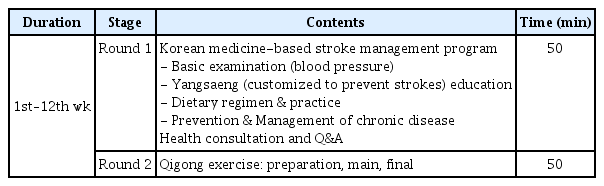
The Korean medicine healthcare program was a 12-week program beginning in May 2018 that was held twice a week for 2 hours at the Y-city health center. The contents of the program were developed by 5 professors of Korean medicine and public health, 1 nutritionist, 2 health and fitness instructors, 2 nurses, and 1 program manager. Each session consisted of a basic examination, education on stroke risk factor management, Korean medicine health preservation “Yangsaeng” education (customized education for strokes including the living environment, sleep, diet, mindset, and exercise), cooking regimen and Qigong exercise. The Yangsaeng education was carried out in Round 1 and Qigong exercise was in Round 2. Yangsaeng (health preservation) is an oriental traditional health management method that promotes health to prevent disease under certain principles with the aim of living a long and healthy life. It is a general concept of the health promotion, disease prevention, immunity enhancement and hygiene in groups of people [21]. Yangsaeng is deeply related to human lifestyle, and implies subjective well-being. It can be classified as morality yangsaeng, mind yangsaeng, diet yangsaeng, activity and rest yangsaeng, exercise yangsaeng, sleep yangsaeng, seasonal yangsaeng and sexual yangsaeng. The Qigong exercise session consisted of a preparation, main, final, and stimulation stage within a safe and effective range of movements considering the age of the participants. Qigong exercise is a method of health preservation which improves physical and mental health by exercising with posture control, breathing exercises, relaxing the mind and body, concentrating and managing consciousness, and rhythmic movements. Qigong has a positive effect on the body and mind, improving psychological stability and mental health [16]. The program also encourages the participants to use their training and exercises daily at home (Table 1).
7. Statistical analysis
The collected data were analyzed using the SPSS/WIN18.0 (SPSS Inc., Chicago, IL, USA) statistical program. The general characteristics of the participants were analyzed by descriptive statistics (percentage and mean). To test for homogeneity, chi-square test, t test, and Mann-Whitney U test were used. The difference between the dependent variables of the 2 groups were measured using ANCOVA with the pretest scores as covariates.
Results
1. Participants’ characteristics and baseline comparison
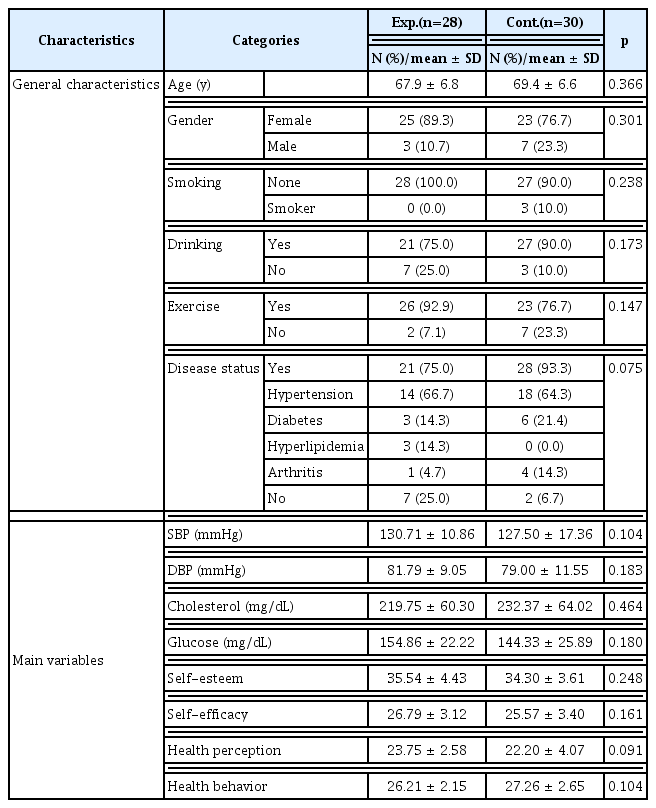
The treatment group and the control group consisted of 28 and 30 participants, respectively. The mean participant age was 67.9 years in the treatment group and 69.4 years in the control group. The treatment group comprised of 25 women and the control group comprised 23 women, which showed a similar distribution. There were more non-smokers than smokers in both groups, and many participants answered “yes” when asked whether they drank alcohol. Many participants in both groups answered that they had diseases and were exercising. Before the program, there were no statistically significant differences between the 2 groups in terms of physiological indices such as systolic BP (p = 0.104), diastolic BP (p = 0.183), cholesterol (p = 0.464), and blood glucose (p = 0.180). In addition, there was no statistically significant difference in terms of self-esteem (p = 0.248), self-efficacy (p = 0.161), health perception (p = 0.091), and health behavior (p = 0.104), which confirmed the homogeneity of the 2 groups (Table 2).
2. Effects of the Korean medicine healthcare program
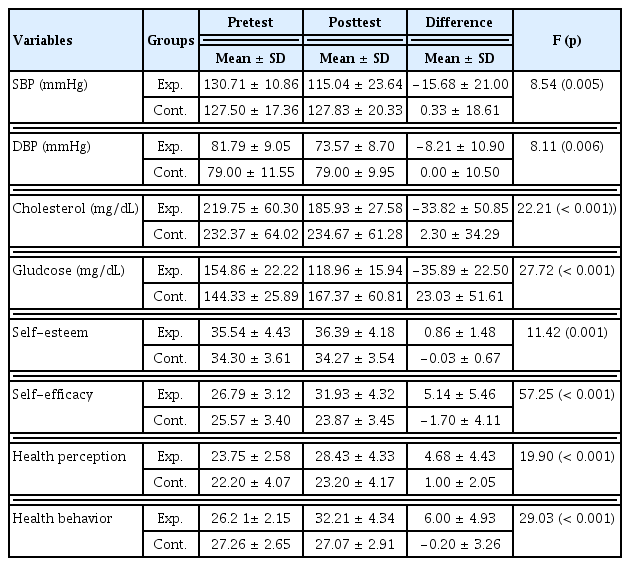
As a result of verifying the physiological indices, there were statistically significant differences in the systolic BP (F = 8.54, p = 0.005), diastolic BP (F = 8.11, p = 0.006), cholesterol level (F = 22.21, p < 0.001), and blood glucose concentration (F = 27.72, p < 0.001) between the 2 groups (Table 3). As a result of verifying self-esteem and self-efficacy, the results showed that there were statistically significant differences in self-esteem (F = 11.42, p = 0.001) and self-efficacy (F = 57.25, p < 0.001) between the 2 groups (Table 3). As a result of verifying health perception and health behavior, the results showed that there were statistically significant differences in health perception (F = 19.90, p < 0.001) and health behavior (F = 29.03, p < 0.001) between the 2 groups (Table 3).
Discussion
The purpose of this study was to examine the effects of the Korean medicine healthcare program for stroke-related factors and self-care enhancements in local community residents. In terms of stroke-related factors, systolic and diastolic BP, cholesterol and blood glucose levels were statistically significantly different. The results in this current study were similar to observations reported by Kim et al [22], in which the systolic BP, diastolic BP, and blood glucose levels of the treatment group showed a significant decrease following secondary stroke prevention education, and a significant difference compared with the control group. The results in this study were also similar to those reported by Shin and Lee [23] in which the high BP group showed higher health preservation scores compared with the normal BP group. This is because the group participants recognized that they had high BP and made an effort to practice healthy lifestyles. Making an effort to prevent the stroke symptoms from worsening is considered a general behavior, while trying to prevent a stroke whilst in a healthy state, is very difficult. In this regard, this current study is meaningful as the participants have not suffered a stroke but they were people at risk of a stroke and had chronic diseases. Thus, it gives more significant meaning to the study that obtained positive effects of physiological indices related to strokes by deriving the changes in health perception and health behavior through Korean medicine. This shows similar results to a study which showed a significant reduction in neutral fat (triglycerides) and blood glucose levels by giving Korean medicine self-help programs to the elderly living alone [21]. This was considered the result of the participants’ continuous health maintenance in everyday life because Korean medicine is easy to understand and approach as an oriental traditional health management method. In addition, health preservation and Qigong exercises are easy to practice. Education alone cannot improve health, there needs to be behavioral changes applied. Therefore, it is necessary to plan and implement interventions using the resources available in everyday life. From this perspective, Korean medicine is easily accessible and effective. BP, blood glucose and cholesterol levels are stroke risk factors that are associated with lifestyle habits. Modifying these potential risk factors before a stroke occurs, reduces the incidence of strokes and the associated secondary disabilities and also reduces financial healthcare spending. Planning and implementation of Korean medicine as an intervention program in everyday life by considering the characteristics of each disease will be advantageous in terms of health promotion and economics.
In addition, the levels of self-esteem and self-efficacy were statistically significantly improved in those individuals who participated in the Korean medicine healthcare program. Although direct comparisons are difficult to make between studies because only a few studies have used Korean medicine programs, a study by Wang et al [21] showed a significant reduction in depression and stress in the elderly living alone, and an increased health preservation by accessing Korean medicine self-help programs. Self-esteem is a factor which refers to the positive perception of oneself and others’ ability [17]. Self-efficacy is a major determinant of changes in human behavior and if there is a personal belief that one can successfully perform the behavior then the desired outcome can be achieved [7]. In terms of stroke patients, self-esteem has been shown to have a significant positive correlation with rehabilitation motivation and competency to perform daily life activities [11]. Self-efficacy has been reported to be closely related to health promotion [8]. That is, one can achieve a goal if there is self-belief which is associated with competency. The improvement of self-esteem is the improvement in the positive perception of one’s ability to manage health. Self-efficacy can lead to changes in health behavior by acting as a driving force for people to continue healthcare activities to prevent strokes. In this study, self-esteem and self-efficacy levels were also improved by using a Korean medicine healthcare program, which led to changes in health perception and health behavior. Therefore, self-esteem and self-efficacy of people in the local community are important as they serve as guidelines for patients and their families to implement in their daily lives through rehabilitation. This study improved self-esteem and self-efficacy using Korean medicine health preservation and Qigong exercise and is very effective. If Korean medicine is used (which has high usability and accessibility) to enhance self-esteem and self-efficacy of participants who have not yet experienced strokes, the risk factors may be reduced and prevent strokes.
The changes in health perception and health behavior increased significantly in the treatment group. This observation was similar to a study where secondary stroke prevention education was the main intervention [22]. Increased exercise performance scores were reported in the treatment group (which was significantly different to the control group), and there were significant differences in the participants’ dietary compliance, non-smoking compliance, daily life compliance, and moderate drinking compliance [22]. Similarly, another study showed a significant increase in self-management performance through arthritis management programs using Qigong exercise [16]. Self-efficacy and stroke health promotion behavior was shown to improve when discharge education programs were used [24]. In this current study, education and Qigong exercise using health preservation, improved the participants’ perception that health problems are related to daily lifestyle, exercise, dietary habits, and weight control. It also brought about changes in behaviors related to health such as regular exercise, reducing salt intake, consuming less fat, eating regular meals, drinking less alcohol, reduced/giving up smoking, weight control, and getting enough sleep. In order to enhance the participants’ symptom management behavior, it is most effective to help them manage themselves by using a cognitive-behavioral approach that includes exercise [25]. Strokes may be prevented by providing education, administering Qigong exercise, and focusing on Korean medicine health preservation. All of which can be used in real life to produce changes in perception and behavior. This implies that Korean medicine programs that are disease specific, will contribute to disease prevention and health promotion.
This study confirmed that the Korean medicine healthcare program using health promotion and Qigong exercise, has a positive effect on stroke associated factors. Thus, Korean medicine can be used actively as an intervention method to prevent disease and promote health. However, the limitation of this study was that participants were residents in the 1 area. Discretion is advised to avoid generalizing the results of this study. Further studies with residents over many areas, with a larger number of participants and more detailed analysis of factors related to strokes would be beneficial, and developing specific Korean medicine intervention programs categorized by disease would be informative.
Acknowledgment
This work was supported by Youngsan University Research Fund of 2019.
Notes
Conflicts of Interest
The authors declare that they have no conflicts of interest.